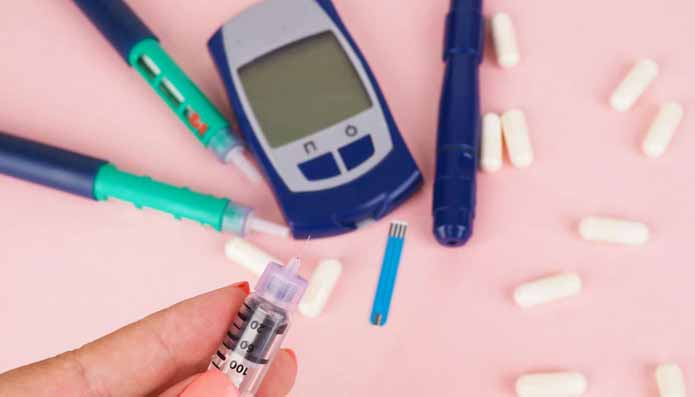
How much should you be prepared to pay for a Medicare supplement for diabetes? What are the limitations? What is the out-of-pocket maximum? How do you know which plan is right for you? Read on to find out! This article will help you find out how much you can expect to pay. You can also get advice from a licensed insurance agent. Listed below are some of the most important factors you need to consider:
Coinsurance

You may wonder: How much do Medicare supplement plans cost? Depending on your income, Medicare will pay for some diabetic supplies and services. However, you may have to pay more for some prescriptions and out-of-network services. To determine if you qualify, review your Medicare supplement plan’s summary of benefits, which will outline the coverage you receive for your diabetes. You can also inquire about discounts available to you, and speak to a licensed insurance agent about what is available.
Part B is medical insurance that covers doctor visits, outpatient care, some preventive services, and medical equipment, including insulin pumps. Medicare covers 80% of most covered services, leaving the patient responsible for the remaining 20%. Part B also covers the Medicare Diabetes Prevention Program, or MDPP, which offers healthy eating and physical activity training to help you lower your risk of diabetes. You may need to pay a coinsurance or a copayment, depending on your income level.
Copayment
You’ve probably wondered, “How much will my health insurance cover for diabetes?” You’re not alone. Many Americans don’t know how to calculate their insurance costs, so we’ve put together this guide to help you get started. This guide will also help you understand the terminology used by insurance companies and the providers. Listed below are some common terms and their definitions. For example, deductible means how much you have to pay before your health insurance will pay for certain services.
The cost of your insulin is determined by your Part D plan’s formulary and tier placement. In 2017, for example, the most expensive insulin was Lantus Solostar. Only half of Part D enrollees paid for it. Another third spent more than that. This is because insulin has a much higher out-of-pocket cost, and Medicare Advantage drug plans tend to cover only two products per class, continue to read here.
Out-of-pocket maximum
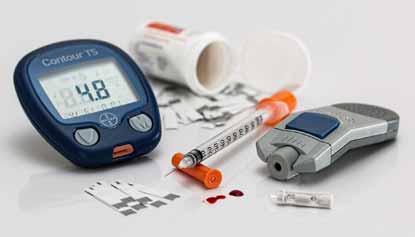
There are several ways to get help paying for your diabetes-related expenses. You can get financial aid from your insurance, local programs, medicine-assistance programs, and other sources. You can also learn how to save money on diabetes supplies. If you are diagnosed with diabetes, you should know that your health insurance plan is required to cover you. It is also illegal for health insurance companies to charge you more for your diabetes because of your pre-existing condition. To get the best possible coverage, you should be aware of key terms and phrases related to diabetes costs.
Original Medicare does not have an out-of-pocket limit. After paying the annual deductible, Medicare will pay the remaining 80 percent of covered diabetic services. Medicare Supplement plans are private insurance companies that administer the program. Some SNPs cover additional services. The out-of-pocket maximum for Medicare supplement for diabetes varies depending on the plan. If you don’t have Medicare, you should choose a Medicare Part B plan. It will cover most of your diabetes medications and treatment costs. You can choose a plan that covers the deductible, coinsurance, and copayments. If you’re under 65, you should choose a Medicare Part B plan.
Conclusion:
Medicare Part B will cover many of the costs of diabetic supplies and services, but you will still be responsible for some out-of-pocket expenses. If you’re covered by Medicare, you may not have to pay a cent. Medicare covers 80% of diabetic supplies and services, leaving you to pay 20%. This is why most people with diabetes have a Medicare Supplement plan or a Medicare Advantage plan. While these plans vary widely in coverage and cost, they all pay after Medicare pays first.